Grading Severity of Aortic Stenosis
Aortic valve stenosis is a serious disease that can lead to heart failure, strokes, and even death if left untreated. That makes timely diagnosis and treatment of the condition crucial. However, treatment of aortic stenosis depends on its severity.
Typically, the following parameters are used to determine the severity of aortic stenosis:
- Pressure gradient – High gradient (HG; >/=40 mm Hg) or low gradient (LG; <40 mm Hg)
- Blood flow – Normal flow (NF; SVi>35 ml/m2) or low flow (LF; SVi<35ml/m2)
- Left ventricular ejection fraction (LVEF) – Preserved (>/=50%) or reduced (<50%)
Depending on the pressure gradient and blood flow parameters, aortic stenosis is graded as follows:
- Normal flow-low gradient (NF-LG)
- Normal flow-high gradient (NF-HG)
- Low flow-high gradient (LF-HG)
- Low flow-low gradient (LF-LG)
NF-HG is the most prevalent type of aortic stenosis and has well-established management protocols. Patients with NF-HG are also ideal candidates for aortic valve replacement. While LF-LG is fairly rare, it’s often associated with a poor prognosis.
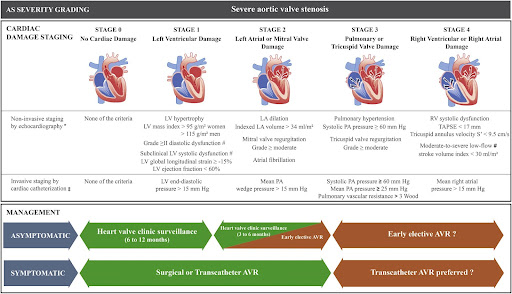
Additionally, depending on progression, heart valve disease can be categorized into the following four stages:
- Stage A (At risk) – Characterised by the presence of risk factors
- Stage B (Progressive) – Mild or moderate valve disease with no noticeable symptoms
- Stage C (Asymptomatic severe) – Severe valve damage with no noticeable symptoms
- Stage D (Symptomatic severe) – Severe valve disease with noticeable symptoms
Doctors use a variety of diagnostic tests to evaluate the aforementioned parameters and determine the severity of aortic stenosis. If you experience symptoms like chest pain, heart murmur, or palpitation, it’s crucial to reach out to an experienced cardiologist and get the right treatment for aortic valve stenosis.
How Does One Diagnose Aortic Stenosis – ECG, ECHO, TEE, or CT aortogram?
Early diagnosis of aortic valve stenosis is crucial to prevent severe complications, such as arrhythmias, heart failure, stroke, and death. Also, it can help administer timely treatment, thus improving the patient’s prognosis and quality of life.
That’s why cardiologists use a series of tests to diagnose aortic valve stenosis and its underlying cause. When you visit the doctor, they’ll start by asking you about your symptoms and medical history. Also, they ask whether your family has a history of cardiovascular ailments. Next, they’ll use a stethoscope to detect the presence of the characteristic aortic stenosis murmur.
Additionally, your doctor will use one or more of the following tests for the complete diagnosis:
- ECG (Electrocardiogram) – It’s one of the most preliminary tests that evaluate the heart’s electrical activity and helps doctors identify an irregular heartbeat and other abnormalities.
- Echo (Echocardiogram) – It uses sound waves to generate images of the beating heart. It helps doctors examine how blood flows through each valve and determine the severity of aortic stenosis.
- TEE (Transesophageal echocardiogram) – It’s a special type of echocardiogram in which an ultrasound probe is inserted into the esophagus and directed closer to the heart. It helps doctors take a closer look at the aortic valve and identify the underlying cause of aortic stenosis.
- CT aortogram – It’s used to evaluate the blood supply to the upper body and identify conditions such as atherosclerosis.
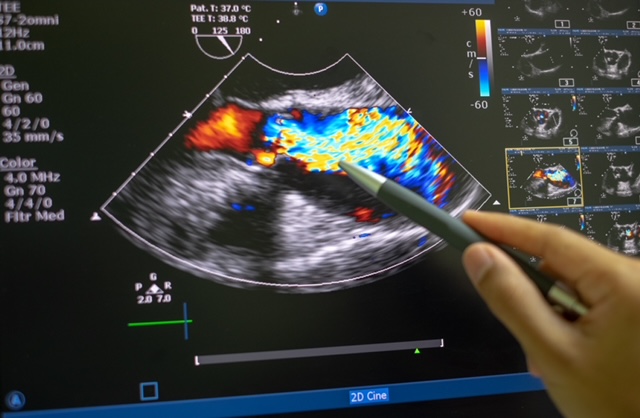
Additionally, your doctor might recommend tests like cardiac catheterization and chest X-ray to get a complete picture of your cardiac health and plan the right course of treatment.

