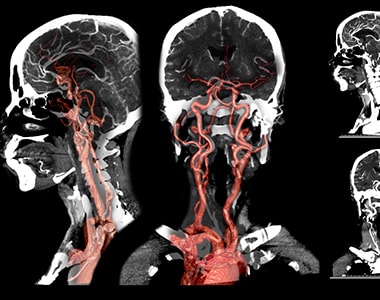
Carotid artery disease is a condition that arises when the fat deposits accumulate and block the blood vessels that deliver blood to the brain.
Peripheral Vascular Disease | Dr Raghu
© 2024, Dr. Raghu. All rights reserved. Design & Developed by AMSDigital.in
+91 95424 75650