Deep Vein Thrombosis
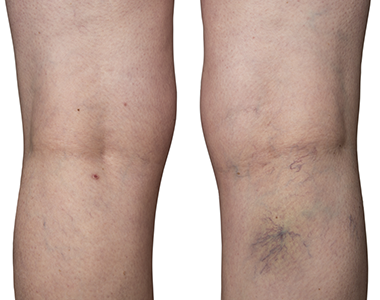
When a blood clot (thrombus) is formed in one or more of the deep veins of your body (usually in the legs), it is known as deep vein thrombosis (DVT). Sometimes this clot becomes detached from the inner walls of the blood vessel and travels to another part inside the body. DVT may develop due to an underlying medical condition particularly the one which affects the clotting of the blood.

Causes and risk factors:
It can be caused by the factors which prevent the normal circulation of the blood and it’s clotting, such as long periods of rest (during a particular medical condition), injury to the vein, surgery and certain medications.
The risk factors are as follows:
- Inherited blood clotting disorder
- Prolonged bed rest
- Surgery
- Pregnancy
- Contraceptives or hormone replacement therapy
- Obesity
- Smoking
- Cancer
- Heart failure
- Inflammatory bowel disease
- Age (usually older than 60 years but can also occur at any age)
Complications:
The following are the complications which may arise due to DVT:
Pulmonary embolism: In Pulmonary embolism, a thrombus present in another part of your body usually a leg, travels to the blood vessel of the lung and blocks the blood circulation, leading to a life-threatening condition.
Post-phlebetic syndrome (post thrombotic syndrome): set of signs and symptoms seen after a blood clot has formed.
Symptoms:
The person may be asymptomatic during the formation of the thrombus, however, during post thrombotic period when it has caused damage to the veins, the blood flow to the affected body part may be compromised. The following symptoms are observed:
- Persistent swelling of the leg or arm (edema)
- Leg pain or tenderness while standing
- Skin discoloration in the affected arm or leg
- Veins in the arm or leg appearing larger than normal
Sometimes the development of a serious health complication such as pulmonary embolism is responsible for the symptoms in the DVT patients which are as follows:
- Shortness of breath
- Chest pain
- Cough (blood may be coughed out as well)
- Back pain
- Profuse sweating
- Lightheadedness
- Blue nails or lips
These symptoms appear suddenly, and an immediate medical attention is required.
Diagnosis:
The diagnosis is initiated by a thorough clinical examination and involves review of the patient’s medical history. Based upon these findings, the physician will categorize the patient into low or high risk DVT. Further tests may be considered to rule out other health problems and to confirm the diagnosis, which are as follows:
- Blood tests: These are considered to evaluate any blood disorders that increase risk of DVT.
- D- dimer test: In this test, the levels of a protein called D-dimer is assessed. In patients with DVT, high levels of this protein can be found in the blood.
- Duplex ultrasonography: It is a non-invasive evaluation of the blood flow in the arteries and the veins of a patient. But this test is not preferred for a thrombus located very deep inside the body such as pelvis.
- Venography: It is a specialized type of an x-ray procedure wherein a dye is injected into a vein of the foot, and the blood clot if present is detected.
- Magnetic resonance imaging (MRI): It is performed in patients for whom ultrasound examination is inappropriate or unfeasible. It can even detect a thrombus present in the patient’s pelvis and the thigh.
Prevention:
A recent World Thrombosis Day Ipsos survey showed that there is less awareness of DVT in countries around the world. Thus, the first step in prevention is making the public aware of DVT. The preventive measures are different depending on the person’s condition who are at risk of developing DVT:
During pregnancy
In pregnant women, certain medication may be prescribed if she has risk factors such as likelihood of having a cesarean birth, bed rest, history of DVT, and inherited thrombophilia.
During travel or in longer hours of sitting posture:
- Drink lots of fluids.
- Wear loose fitting clothes.
- Walk and stretch at regular intervals.
- Use special stockings to improve blood flow and to prevent blood clots but consult your health care provider before using it.
Treatment:
Treatment for DVT includes certain medicines and therapies, which are as follows:
Medications:
- Anticoagulants: They prevent further formation of blood clots but don’t dissolve the already existing ones. Most common anticoagulants used are heparin and warfarin. Warfarin is not recommended during pregnancy.
- Thrombin inhibitors: These are recommended for people who can’t take heparin.
- Thrombolytic medicines: These are recommended only during life threatening condition.
Compression stockings:
It may be recommended to prevent swelling and to avoid post-thrombotic symptoms in the patients.
Surgical treatment:
Surgical treatment may be performed when medications fail to dissolve the clots.

