Primary Angioplasty – Heart Attack Symptoms
What is a Heart attack?
- A heart attack is a life-threatening condition, where the heart is not receiving enough oxygen because the blood supply is blocked.
- It happens due to building up of cholesterol plaque in the coronary arteries (Blood vessels supplying the heart).
- This interrupted blood flow can destroy or damage the part of the heart muscle.
- A heart attack is also known as myocardial infarction or acute coronary syndrome.
What are the symptoms of a heart attack?
- Chest discomfort
- Shortness of breath
- Palpitations
- Pain in the neck muscles, shoulders, lower jaw, arms, abdomen or upper back
- One can experience symptoms like Lightheaded, dizzy or faint
- Fatigue
- Nausea or vomiting
- Unusual sweating
- Anxiety

Who are at risk of developing a heart attack?
Patients with the following risk factors may have a higher incidence of heart attack
- Elderly age
- Atherosclerosis
- Elevated cholesterol levels
- High blood pressure
- Diabetes
- Smoking
- Family history of heart attack
What are the complications of a heart attack?
- Heart failure
- Cardiac arrest
How is a heart attack diagnosed?
- Electrocardiogram
- Biomarkers – Highly sensitive troponin
- Chest X-ray
- Echocardiogram
- Coronary angiogram
What needs to be done if one has a heart attack?
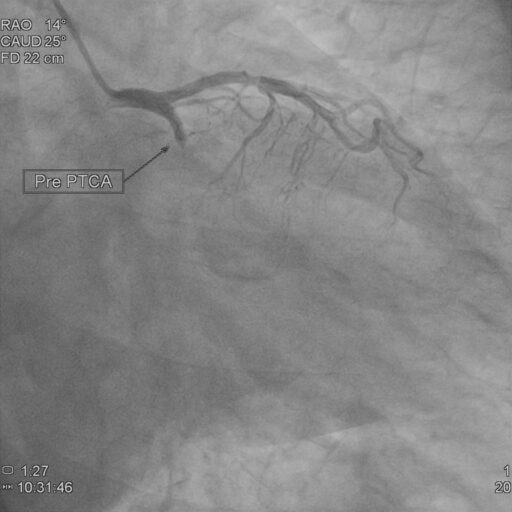
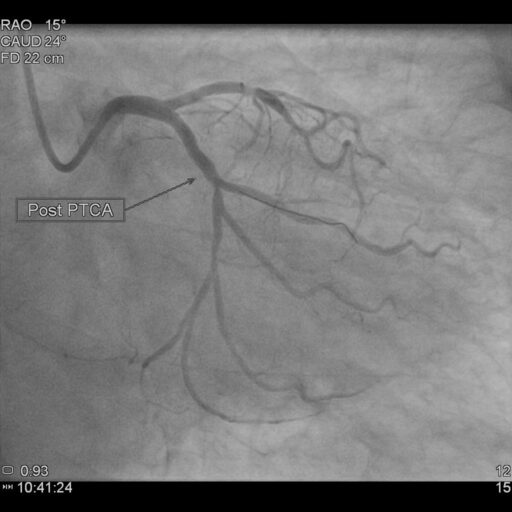
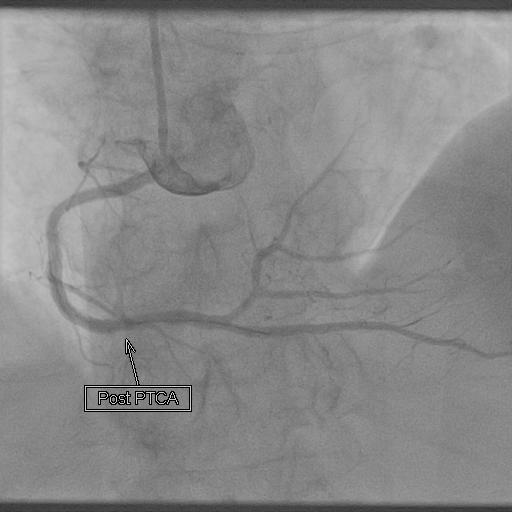
- Many patients who have a heart attack will either go for primary angioplasty, where the blocked artery is reopened or thrombolysis, where clot-dissolving medicines (thrombolytic agents/ anti-coagulants) are given to restore normal blood flow to the heart.
- Primary angioplasty:
- Primary angioplasty is a procedure that uses a balloon catheter or stent to treat obstructed/narrowed/blocked coronary arteries to improve blood flow to the heart.
- The coronary arteries are usually blocked by cholesterol plaque (deposits) in the artery wall that causes decreased blood flow and leads to heart attack
- This is a preferred procedure for heart attack as soon as symptoms start
Why timelines are important during a heart attack?
- Delay in the treatment delivery between the onset of symptoms and primary angioplasty leads to severe damage to the heart muscle.
- Primary angioplasty needs to be done within 60 minutes after arrival at the hospital.
- In the case of angioplasty, the facility is unavailable, a medicine to dissolve the blood clot (Thrombolytic agent) can be administered. If thrombolysis is planned it should be started within 10 minutes after arrival at the hospital.
- An ECG should be taken and interpreted within 10 minutes after arrival at the hospital.
- For every 15 minutes of delay in performing angioplasty after 90 minutes of arrival to the hospital the risk of death doubles.
What are the complications of primary angioplasty?
- Repeat heart attack
- Stroke
- Kidney damage
- Rupture of the coronary artery
Understanding the procedure
Before the procedure:
- List all the current medications and supplements used
- Any allergies towards the medications should be reported
- Blood samples are taken for clinical investigations
- Vitals are checked
- Electrocardiogram and 2D echo is done
- Stop heavy meals or processed food before 8 hours of the procedure
- Plan to have someone beside you to take to home after the procedure
During the procedure:
- A patient will be allowed to lie on the X-ray table and strapped
- An intravenous cannula will be inserted
- Electrodes may be placed over your chest to monitor for vitals during the procedure
- Local anaesthesia at the catheter insertion site to make the area numb.
- An incision is made in a wrist or groin area, and small thin flexible tube (catheter) with a small inflatable balloon at its tip is passed into the artery and guided towards the heart
- Contrast dye is injected into the catheter to make coronary arteries to be visible in X-ray
- The catheter is directed towards the blockage until the tip of the catheter lies inside the blocked part of the coronary artery
- A stent which is in position on the balloon will be inserted into the artery and when the balloon is inflated, the stent will expand which will flatten the artery wall by squeezing the cholesterol plaque that improves the blood flow to the heart
- Once the procedure is completed, the catheter is removed with leaving expanded stent inside the artery to hold it open and a bandage is placed over a procedure site.
After the procedure:
- Vitals such as Blood pressure, heart rate, temperature, respiration rate, blood oxygen level will be monitored.
- A patient will be instructed to rest in the ICU for 24 hours.
- Patient hospital stay will be for about a week.
- If the catheter insertion is at the groin, you may be asked not to bend or cross your legs for 12 hours.
- Infections and bleeding manifestations are checked at the procedure site.
- It is very important to take plenty of liquids that keep you hydrated as well as wash off contrast from the body. Accumulation of contrast leads to kidney damage.
- Blood tests, Electro Cardio Gram (ECG), Echocardiogram will be done.
Blood thinners
- It’s important to closely follow doctor’s recommendations about your treatment with blood-thinning medications — aspirin and Clopidogrel or similar medications.
- Most people who have undergone primary angioplasty with or without stent placement will need to take aspirin indefinitely. Those who have had stent placement will need a blood-thinning medication, such as Clopidogrel, for six months to a year. If you have any questions or need any other type of surgery, talk to a cardiologist before stopping any of these medications.
- Primary angioplasty greatly increases blood flow through the previously narrowed or blocked coronary artery. Chest pain generally should decrease and may be able to exercise better.
- Having angioplasty and stenting doesn’t mean heart disease goes away.
- One needs to continue healthy lifestyle habits and take medications as prescribed by a doctor.
- In case of symptoms similar to those before your procedure, such as chest pain or shortness of breath, contact doctor soon.
- Chest pain at rest or pain that doesn’t respond to Sorbitrate, call for emergency medical help.
After discharge from hospital:
Call your doctor’s office or hospital staff immediately if:
- The site where the catheter was inserted starts bleeding or swelling
- Develop pain or discomfort at the site where the catheter was inserted
- Signs of infection, such as redness, swelling, drainage or fever
- There is a change in temperature or colour of the leg or arm at the procedure site
- One can experience symptoms like fainting or weakness
- Develop chest pain or shortness of breath
Lifestyle modifications:
- Quit smoking
- Eat a healthy diet that is low in saturated fat
- Maintain a healthy weight
- Control other conditions, such as diabetes, high blood pressure, and high cholesterol levels
- Get regular exercise
Take medications as prescribed by a doctor
Our Specialities
- Conditions
- Acute limb ischemia
- Chronic limb ischemia
- Aortic stenosis
- Mitral valve stenosis
- Mitral valve regurgitation
- Atrial fibrillation
- Tachycardia
- Bradycardia
- Palpitations
- High blood pressure
- Atrial septal defect
- Ventricular septal defect
- Patent ductus arteriosus
- Cardiac amyloidosis
- Hypertrophic cardiomyopathy
- Varicose veins
- Deep vein thrombosis (DVT)
- Myocarditis
- Endocarditis
- Pericarditis
- Peripheral arterial disease
- Pulmonary artery hypertension
- Pulmonary embolism
- Cath lab procedures:
- Coronary Angiogram
- Primary Angioplasty
- Coronary Angioplasty
- CHIP Angioplasty
- Aortic valve replacement surgery
- Mitral valve replacement surgery
- Device closure for Atrial septal defect
- Device closure for Ventricular septal defect
- Device closure for Patent Ductus Arteriosus
- Transcatheter aortic valve replacement (TAVR)
- Inferior vena cava (IVC) filter
- LA appendage closure
- Fistuloplasty
- Balloon mitral valvotomy
- 24 hours emergency services
- Clinics- weekly basis/monthly basis/ Yearly basis
- Prevention of cardiovascular diseases
- Diagnosis
BOOK AN APPOINTMENT

Dr. RAGHU | Angioplasty Expert in India
Cardiology Coronary, Vascular and
Structural Interventions
Conditions & Diseases
Angioplasty
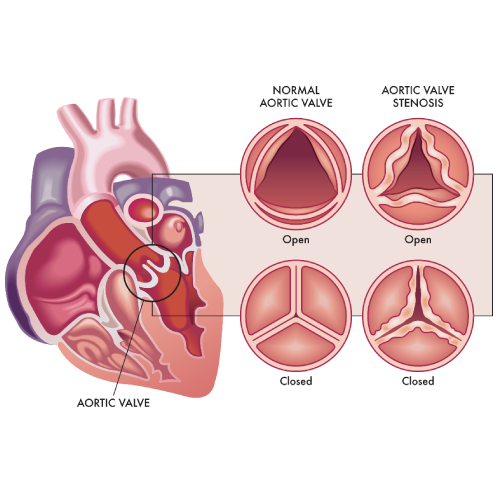
Aortic Stenosis
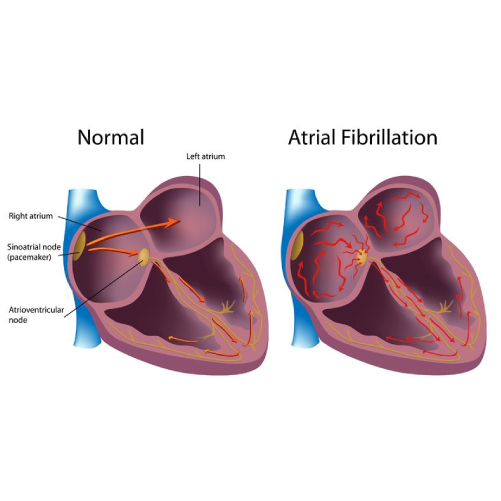
Atrial Fibrillation
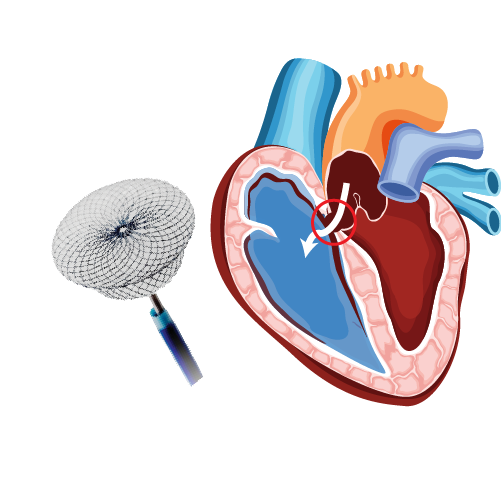
Atrial Septal Defect
+91 95424 75650
© 2024, Dr. Raghu. All rights reserved. Design & Developed by AMSDigital.in

