Atrial Fibrillation- New Therapies in 2022
Introduction
Atrial Fibrillation is a chaotic, irregular beating of the heart. When the heart beating is irregular there will be stasis or stagnation of the blood within the heart chambers. When there is stagnation of blood within heart chambers this will lead to clotting of the blood and these blood clots can get dislodged and land up in the brain leading to a brain stroke so in the treatment of Atrial Fibrillation there are two important strategies both have to be done.
Control or Treat Atrial Fibrillation
First strategy is to control the Atrial Fibrillation or treat the Atrial Fibrillation. Control or treatment of the Atrial Fibrillation is by the use of medications which can control the rate like Beta blocker, Calcium blocker, amiodarone etc so that we can bring back Atrial Fibrillation to a normal sinus rhythm. These drugs that convert the rhythm from an arrhythmia to normal are called anti-arrhythmic drugs. The challenge with the prolonged use of these anti arrhythmic medicines is the high incidence of side effects.
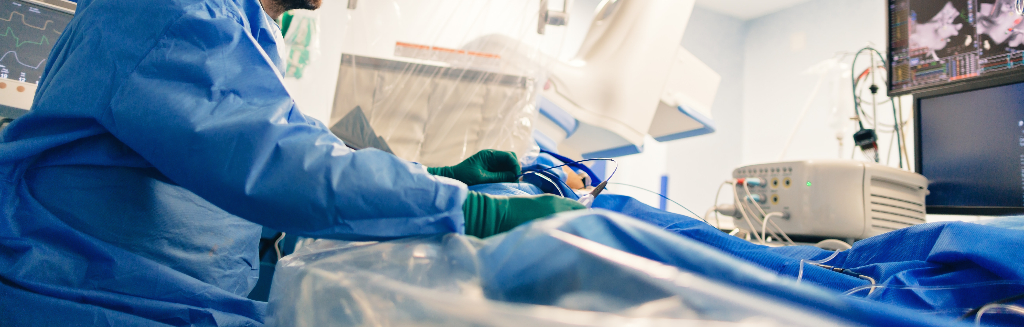
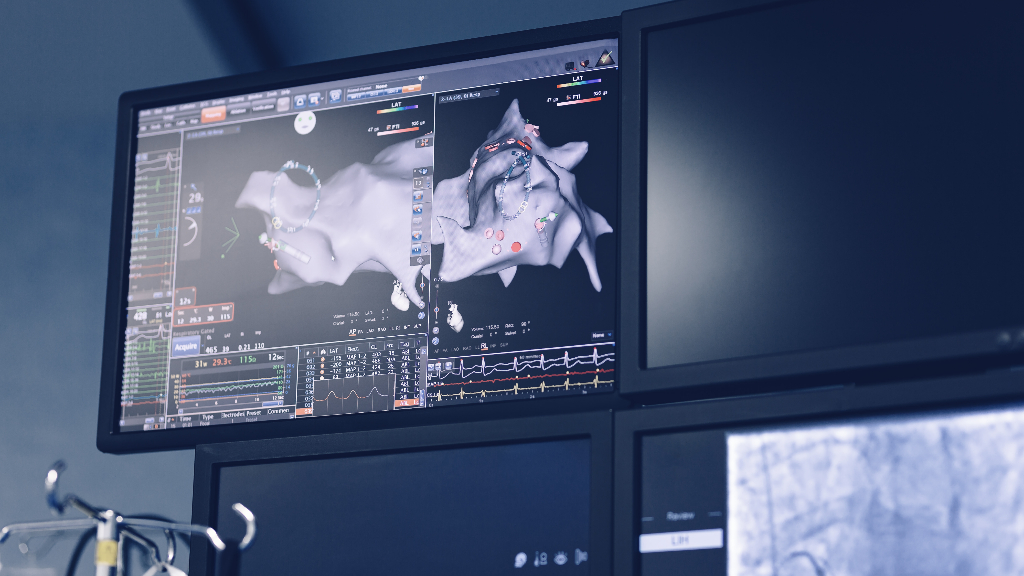
Electrophysiological study and catheter ablation
The other option what has evolved in the treatment of Atrial Fibrillation is the electrophysiological study and catheter ablation. In this therapy what we do is map the focus or location from where the Atrial Fibrillation is originating. Once the focus or the site of origin of the Atrial Fibrillation has been identified then electrophysiologists isolate the location of this irregular heart beat and isolate it from the rest of the heart. So they will create pockets or islands of chaotic beating which are separated from rest of the heart tissue. So in effect these micro pockets are isolated and cannot communicate with the heart’s electrical system.
Over the last three years, a lot of data which has been generated which showed that patients with Atrial Fibrillation when they undergo Catheter Ablation they were doing much better in the form of reduction in the death rate, reduction in the hospitalization rate, reduction in the heart failure and the quality of life is also much better when they undergo a Catheter Ablation.
Prevention of brain stroke
The second strategy which has to be adopted in a patient with Atrial Fibrillation is for the prevention of brain strokes. The most dreaded complication in Atrial Fibrillation is development of brain stroke so to prevent the development of brain stroke the patient needs to take anticoagulants.
Anticoagulants means – coagulation means blood clot; anti means opposite – so those medicines which act against the blood clot are anticoagulants. Life long anticoagulation is needed even when the atrial fibrillation is present for a limited duration.
Vitamin K antagonists
For the past five decades, we have the Vitamin K antagonists like Acenocoumarol or the Warfarin for the prevention and propagation of blood clot formation. These medicines act via blocking Vitamin K which plays a pivotal role in the blood coagulation and are termed Vitamin K antagonists. Warfarin and Acenocoumarol both have been used extensively with good results. They were effective in preventing the stroke but the main challenge with these older generations of Anticoagulants is the increased chances of bleeding with the Vitamin K Antagonist.
Novel or Direct-acting Oral Anticoagulant medicines
To overcome the problem of increased bleeding over the last 8 to 10 years we have three novel oral anticoagulants or direct acting oral anticoagulants (in short they are called NOAC or DOAC).
They have been used to prevent the formation and extension of blood clots within the atrium. Examples of these drugs include – dabigatran, rivaroxaban, apixaban and edoxaban. These are the different types of novel oral anticoagulants which are available in the market.
Advantages of Novel or Direct-acting Oral Anticoagulant medicines
Compared to the previous generation of Warfarin and Acenocoumarol have a much lower risk of bleeding. They are as effective as vitamin K antagonists for the prevention and propagation of blood clots. So in the current day, the standard of care for the prevention of brain stroke in fibrillation is with the direct acting agents – Dabigatran, Apixaban or Rivaroxaban.
Left Atrial Appendage Occluder (LAAO)
The third type of therapy which is used in the treatment of Atrial Fibrillation for prevention of blood clots is the left atrial appendage occluder.
So what is this left atrial appendage occluder?
We already understood that those patients who have got Atrial Fibrillation have an ineffective heart beating ability. So there is stasis of blood clot there.
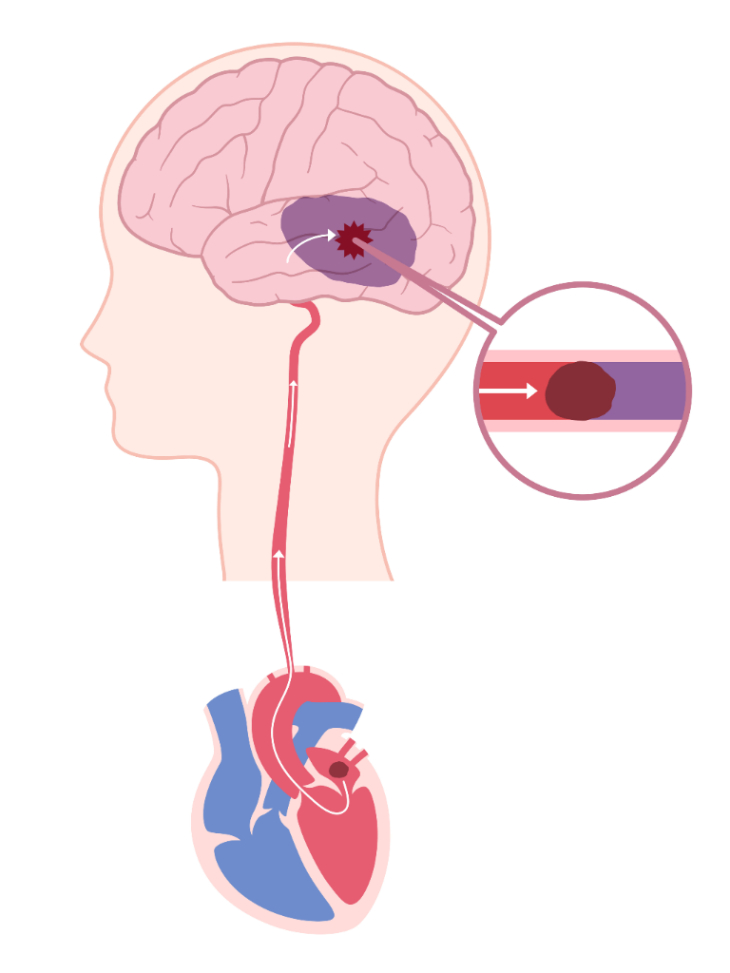
So where is the blood clot happening?
The blood clots are happening in the left atrium. In the left atrium there is a finger shaped structure called the left atrial appendage. There is no real major function of the left atrial appendage but this appendage is a very important focus for the development of blood clots. Nowadays what the cardiologists are doing is block the left atrial appendage by using a left atrial appendage occluder. Till date left atrial appendage was being occluded at the time of surgery by applying a suture.
Left atrial appendage occluder is very useful for those patients
- Who cannot tolerate oral anticoagulants,
- Have a high risk of bleeding of over anticoagulation
- People who refuse to take anticoagulation or
- Patients who cannot be relied upon to consistently take anticoagulation and
- Patients who are at a high risk of having thrombotic or embolic complications because of the Atrial Fibrillation those are the groups.
- Person who is already on anticoagulation still develops a brain stroke
- Recent catheter ablation and electrical isolation
So in conclusion left atrial appendage occluder is an elegant therapy for those patients who cannot tolerate anticoagulants, who have got contraindications for anticoagulant use.

