Diagnosing Atrial Fibrillation and Preventing Stroke
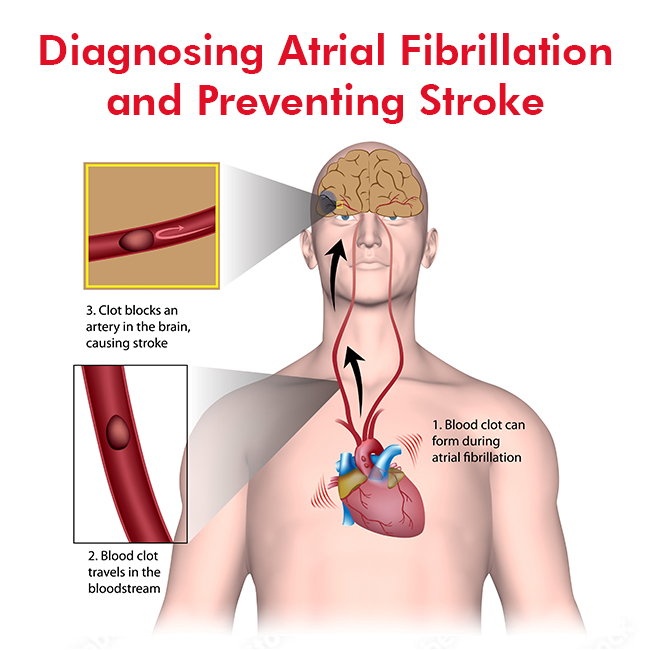
Atrial fibrillation (AFib) interferes with the normal functioning of the heart. It can lead to blood clots, which, in turn, can result in a stroke or heart failure. That makes it crucial to diagnose the condition early on and start the necessary treatment.
If you have been experiencing symptoms like palpitations, dizziness, fatigue, and shortness of breath, it’s important to consult a medical practitioner.

What to Expect When You Visit a Doctor?
If you think you’re at risk of developing AFib or already have the condition, your doctor will ask you about your medical history and symptoms. It’s a good idea to maintain a list of any unusual symptoms you might have been experiencing. If you have pre-existing medical conditions, such as hypertension, coronary artery disease, congestive heart failure, and diabetes, make sure you let the doctor know.
Additionally, the doctor might ask questions about your family history and lifestyle. Once they have the necessary information, they’ll order one or more of the following tests before diagnosing AFib.
Blood Tests
These include tests to check your kidney, liver, and thyroid function. They’ll help identify underlying conditions, like hyperthyroidism, that might be causing afib episodes. Also, they’ll help your doctor decide the right course of AFib treatment.
Periodic ECG especially during palpitations is immensely helpful to diagnose AFib.
Chest X-Ray
It’ll help identify conditions, such as COPD and heart failure, that could be causing AFib.
Electrocardiogram (ECG)
It helps monitor the heart’s electrical activity and detect any abnormalities in the heart rate and rhythm.
Exercise Stress Test
It involves undergoing an ECG while exercising on a treadmill or stationary bicycle. It helps identify conditions like coronary artery disease.
Echocardiogram (Echo)
It generates detailed images of the heart’s structure and movement to help doctors identify faulty valves and other defects.
Long-term ECG monitoring devices introduced in recent times for the diagnosis of infrequent brief episodes of AFib
Portable Heart beat Monitoring
Your doctor might ask you to wear a portable device, like a Holter monitor or cardiac event recorder, to monitor brief and infrequent AFib episodes.
If you don’t have any noticeable symptoms but are worried that you might be at risk of developing afib in the future, you can talk to your doctor about getting screened for the condition.
Stroke is a debilitating consequence of AFib. People who benefit from anticoagulants can be identified by CHA2DS2-VASc score.
Stroke Prevention and Atrial Fibrillation
Experts believe that AFib is responsible for at least 20% of all strokes. Also, it can increase your risk of having a stroke by up to five times. If you’ve been diagnosed with the condition, it’s crucial that you talk to your doctor about stroke prevention.
Risk Assessment
The first thing a doctor will do is evaluate your risk of stroke. They calculate the CHA2DS2-VASc score, which is an acronym for:
- C: Congestive heart failure
- H: High blood pressure
- A: Age 75 and older
- D: Diabetes
- S: Previous stroke
- V: Vascular disease
- A: Age 65 to 74
- Sc: Sex
Anticoagulant Medications
Depending on your score, the doctor might prescribe anticoagulants or blood thinners to prevent the formation of blood clots. While warfarin used to be the most commonly used anticoagulant, doctors now prescribe other drugs like:
- Apixaban (Eliquis)
- Dabigatran (Pradaxa)
- Rivaroxaban (Xarelto)
Surgery
If you can’t take blood thinner due to any medical condition, you can undergo a procedure called left atrial appendage closure to minimize your risk of stroke due to AFib.
Timely diagnosis and proper treatment can improve the quality of life and longevity of individuals with AFib. If you experience any symptoms of AFib, make sure you immediately consult a doctor.

