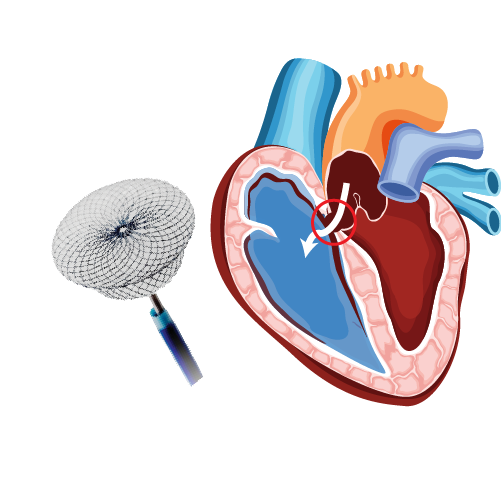
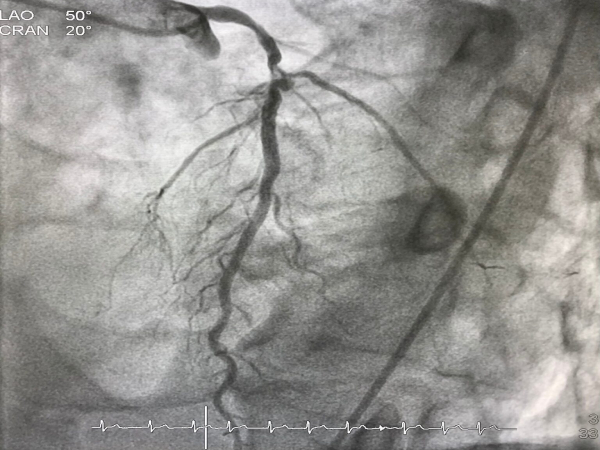
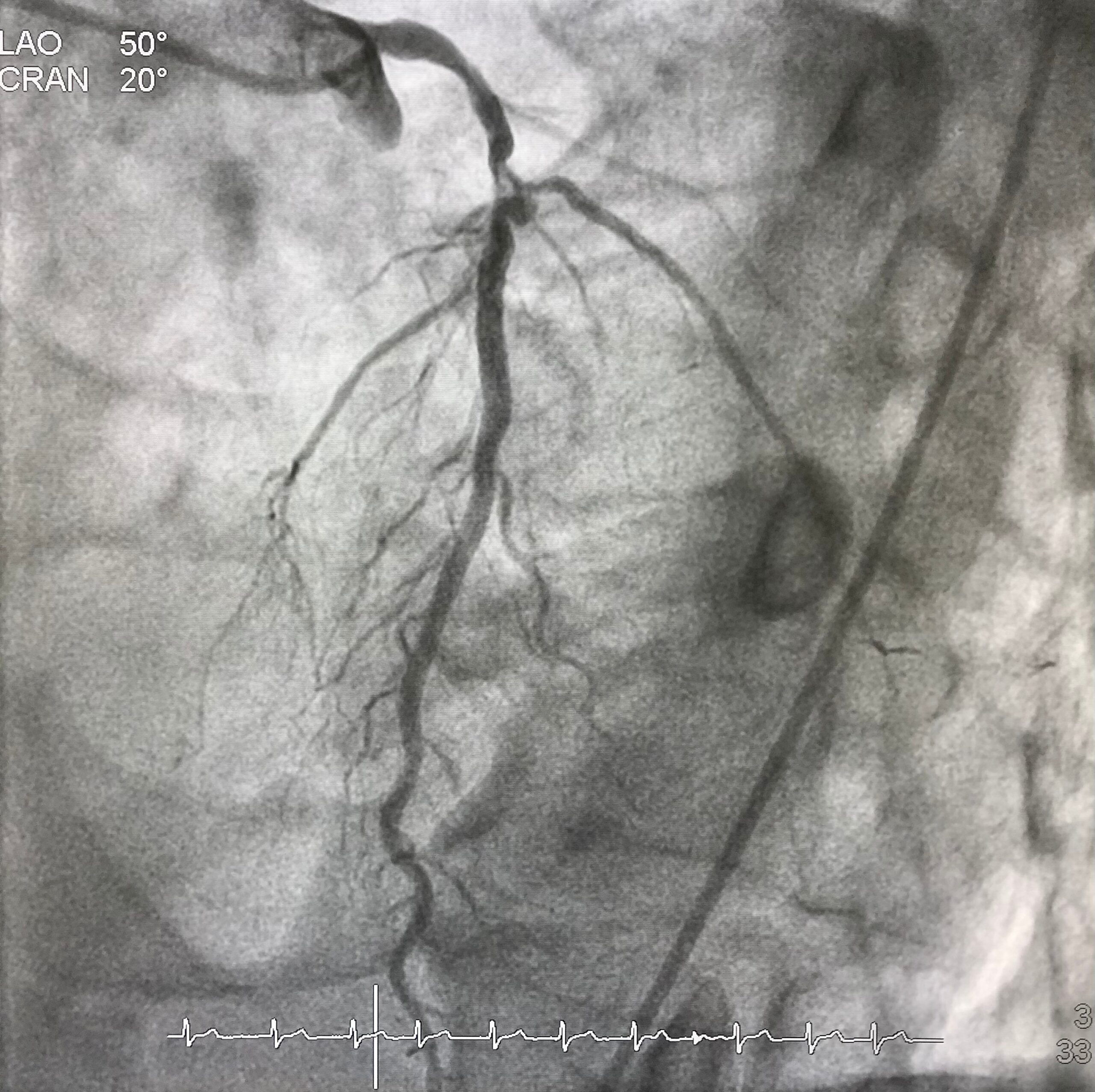
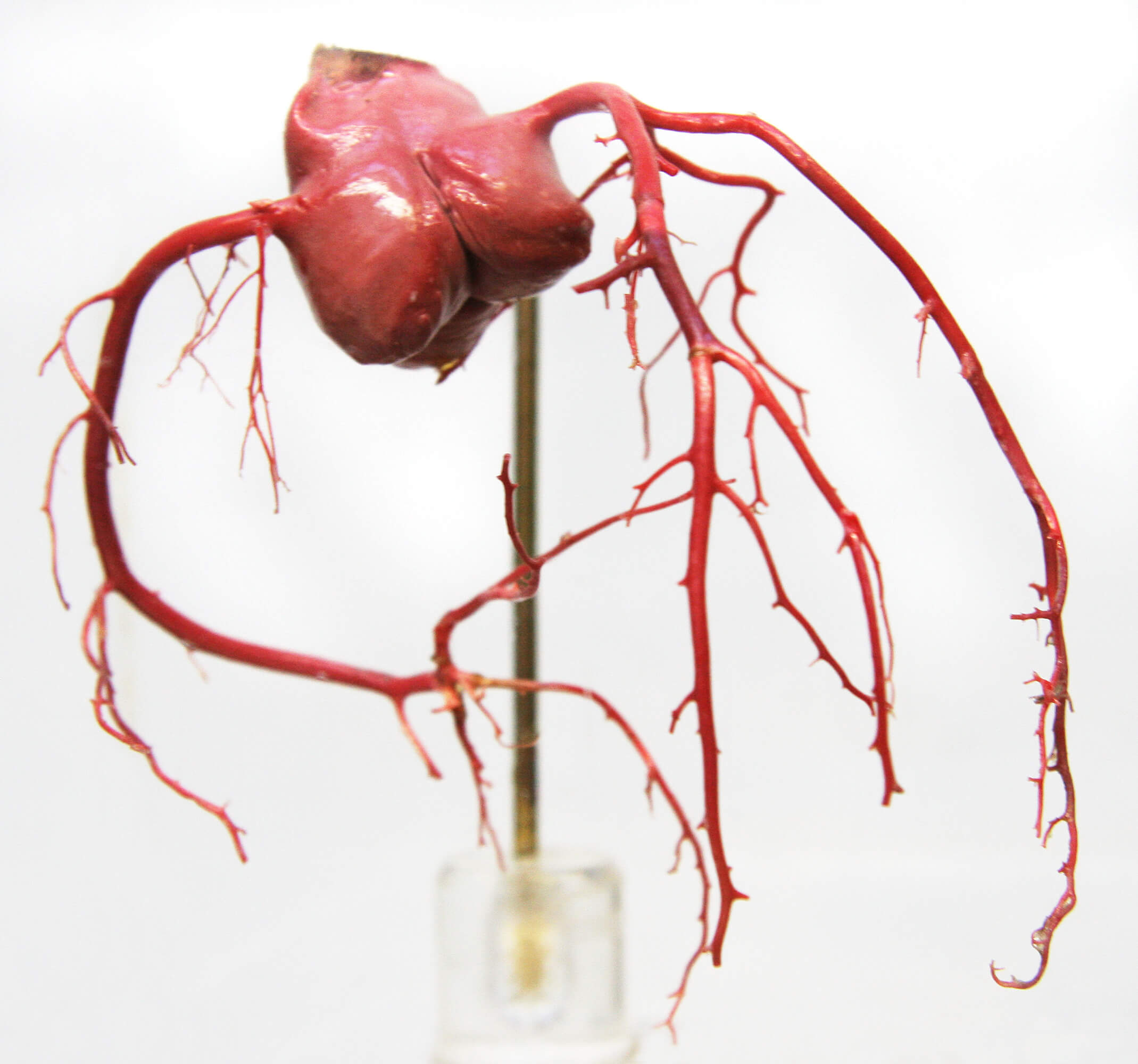
Many people have heart disease, but not all of them know it. Doctors use a variety of tests to identify cardiac ailments and their underlying causes. Coronary angiography is one of the most common diagnostic tests that doctors use.
While it’s considered a safe and minimally invasive procedure, coronary angiography comes with a few risks. You can read more about the potential risks and complications in our previous blog.
The good news is that you can avoid side effects with proper care after the procedure. If you’ve recently had coronary angiography or are going through one soon, here is what you need to do after the procedure:
Avoid Heavy Physical Activity
It’s important to rest after coronary angiography. Avoid lifting heavy objects or resuming your exercise routine right after the procedure. Make sure you get plenty of sleep and let your body and mind relax for at least a week after angiography. Ask your doctor if you’re unsure when to hit the gym or start exercising.
Embrace Healthy Habits
Avoid cigarettes for at least a few days if you are a smoker. Smoking can cause spasms in the coronary arteries, leading to a heart attack or stroke after your angiography. Also, avoid alcohol consumption, and make sure you eat a balanced diet.
If you are a coffee drinker or have high blood pressure, avoiding all caffeine products (coffee, tea) and salt for several days following your procedure may be a good idea. The most important thing is to listen carefully to what your doctor tells you about caring after coronary angiography to avoid any other complications during recovery or later down the road.
Be Careful About Removing the Bandage
A crucial step to caring after coronary angiography is to avoid removing the bandage until the morning of the second day after the procedure. Also, you should not remove it yourself. Let someone else help you remove it. You must consult your doctor or nurse before removing the bandage.
Expect Soreness and Pain for a Few Days
Your arm or leg (where the catheter was inserted) might feel sore for a few days following a coronary angiogram. The discomfort you feel is usually caused by the catheter or dye used for the test.
The catheter may have been left in place too long, leading to irritation and inflammation. Or it could be a reaction to the dye that was used to take images of your arteries during the procedure. It can also happen if you’re allergic to any component of either one.
In most cases, the pain and soreness should subside after a few days. If the pain persists or the arm/leg becomes numb, it’s a good idea to reach out to your doctor. Also, if you have a fever or trouble breathing, call your doctor right away.
If you are bleeding from the incision site, apply direct pressure with a gauze dressing until the bleeding stops. Don’t remove the dressing unless instructed by medical staff at the hospital.
Conclusion
Coronary angiography is a safe and effective procedure that can give you a better understanding of your heart health. If you follow your doctor’s instructions, you’ll be on the road to recovery in no time.
Dr. C Raghu is a renowned cardiologist who has treated thousands of patients with cardiac ailments. If you have any concerns or questions about coronary angiography, feel free to reach out to Dr. Raghu today.
Book Online Consultaion
Care After Coronary Angiography – Blog
Subscribe the Hearty Life Blogs

DR. RAGHU
Cardiology Coronary, Vascular and
Structural Interventions
Conditions & Diseases
Angioplasty
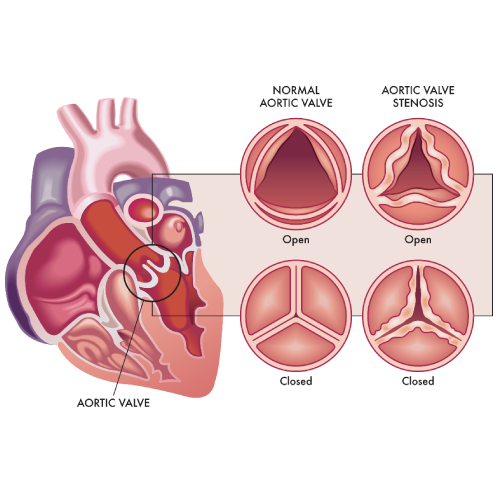
Aortic Stenosis
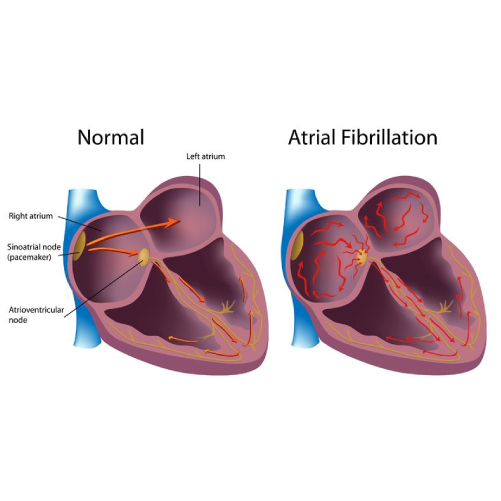
Atrial Fibrillation