Congenital heart diseases are diseases that are present from birth and affect the normal heart functioning. These are the most frequently occurring congenital disorder, responsible for 28% of all congenital birth defects. The birth prevalence of CHD is reported to be 8-12/1000 live births. Considering a rate of 9/1000, about 1.35 million babies are born with CHD each year globally. In most cases, no obvious cause of congenital heart disease is identified. However, some things are known to increase the risk of the condition, including: Many cases of congenital heart disease can be diagnosed before a baby is born during an ultrasound scan in pregnancy. At times a focused foetal heart scan called foetal echocardiography in specialized centers helps to diagnose the cardiac problem before birth. However, it’s not always possible to detect congenital heart defects in this way. Congenital heart disease can have a number of symptoms, particularly in babies and children, including: These problems are sometimes noticeable soon after birth, although mild defects may not cause any problems until later in life. There are many types of congenital heart disease and they sometimes occur in combination. Some of the more common defects include: Treatment for congenital heart disease usually depends on the defect you or your child has. Mild defects, such as holes in the heart, often don’t need to be treated, as they may improve on their own and may not cause any further problems. Surgery or interventional procedures are usually required if the defect is significant and causing problems. Modern surgical techniques can often restore most or all of the heart’s normal function. However, people with congenital heart disease often need treatment throughout their life and therefore require specialist review during childhood and adulthood. This is because people with complex heart problems can develop further problems with their heart rhythm or valves over time. Most surgery and interventional procedures aren’t considered to be a cure. The affected person’s ability to exercise may be limited and they may need to take extra steps to protect themselves from getting infections. It’s important that a person with heart disease and their parents or carers discuss these issues with their specialist medical team.
What are the Causes of Congenital Heart Defects?
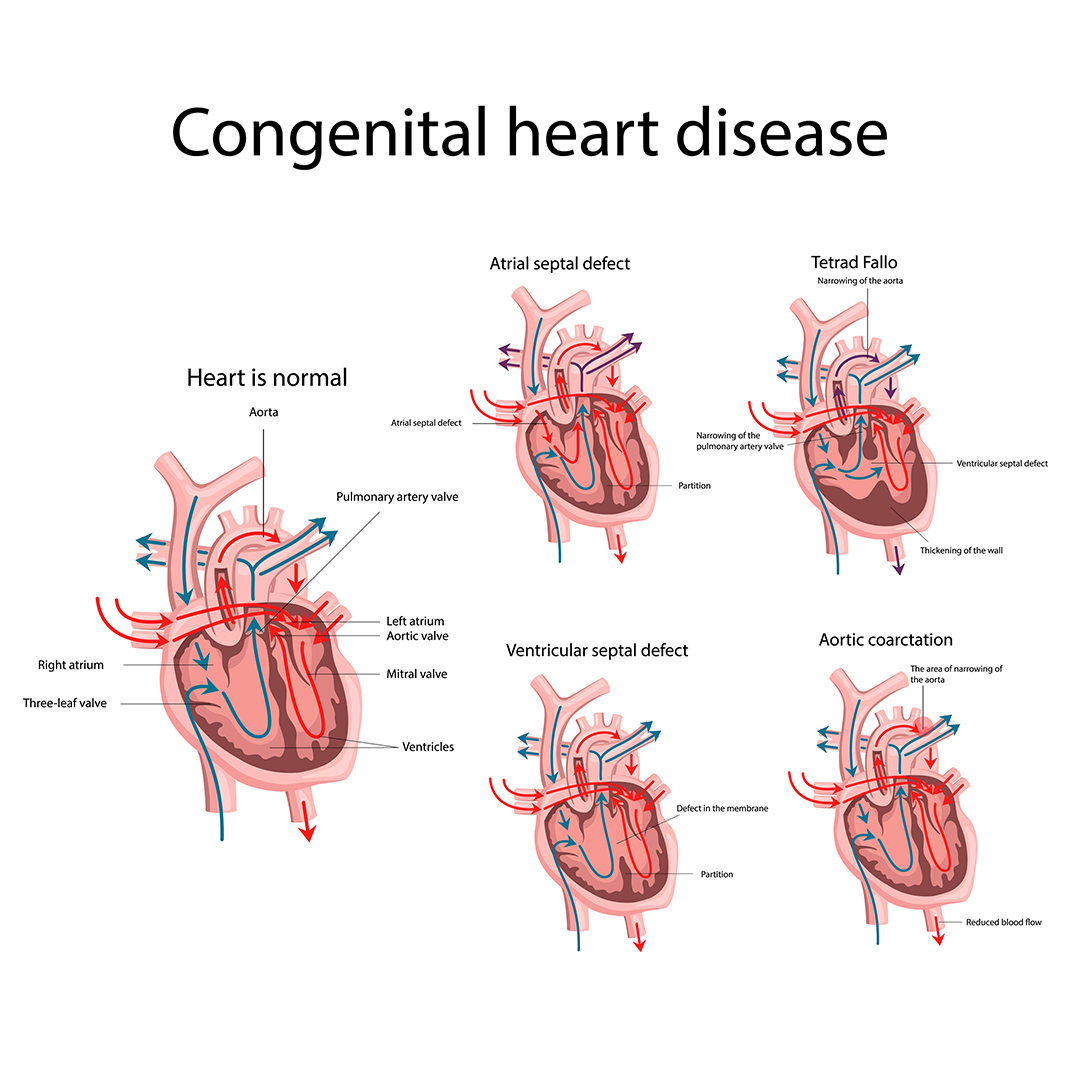
Signs and Symptoms of Congenital Heart Disease
Types of Congenital Heart Disease

Treating Congenital Heart Disease
Book Online Consultaion
Basics of Congenital Heart Disease Blog
Subscribe the Hearty Life Blogs

DR. RAGHU | Best Cardiologist in Hyderabad
Cardiology Coronary, Vascular and
Structural InterventionsConditions & Diseases
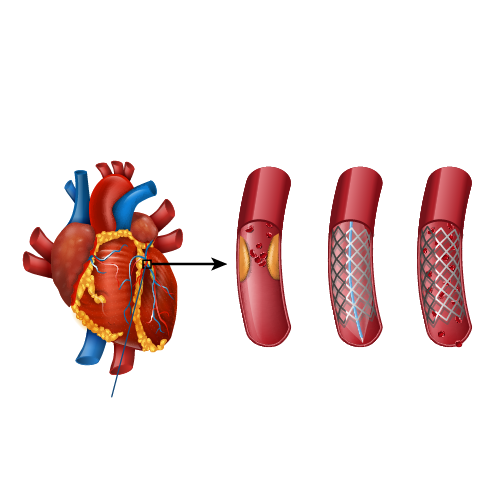
Angioplasty
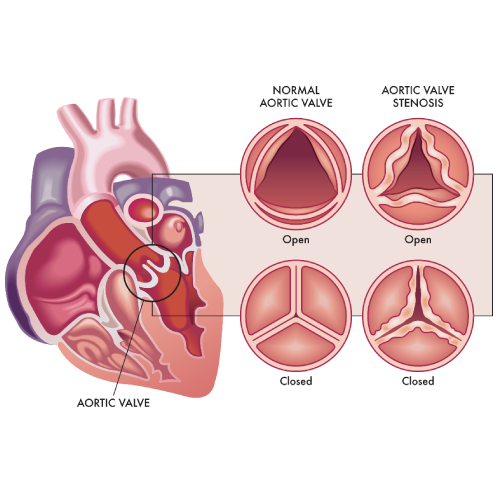
Aortic Stenosis
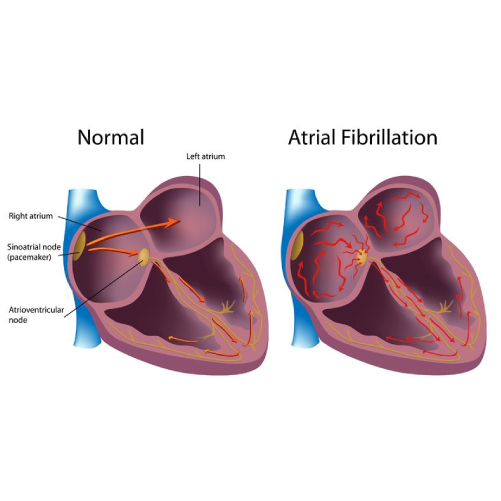
Atrial Fibrillation
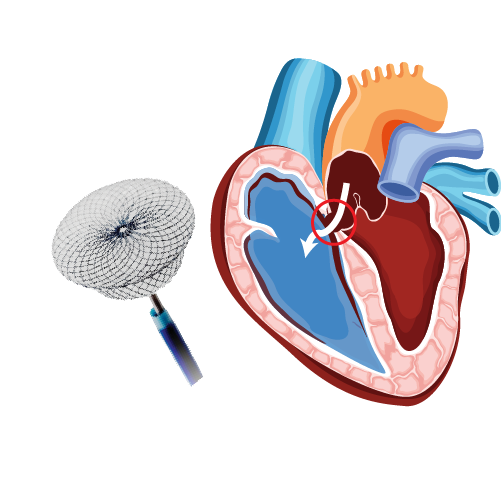
Atrial Septal Defect
Congenital Heart Disease | Dr Raghu
© 2024, Dr. Raghu. All rights reserved. Design & Developed by AMSDigital.in
+91 95424 75650

