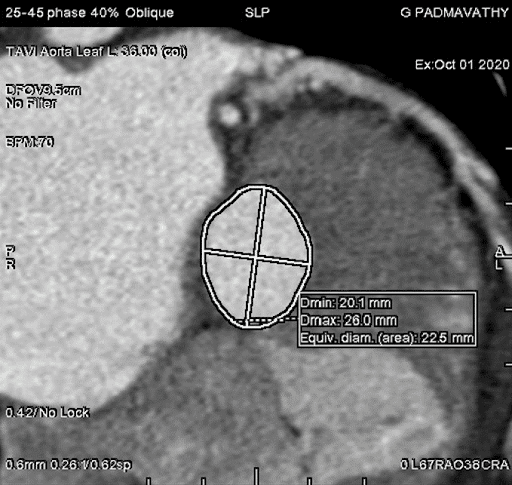
Before you undergo TAVR, your cardiologist will recommend various diagnostic tests to assess your overall health and risk factors. One of the most common tests that doctors prescribe is a CT angiogram.
Aortic Disease | Dr Raghu
© 2024, Dr. Raghu. All rights reserved. Design & Developed by AMSDigital.in
+91 95424 75650