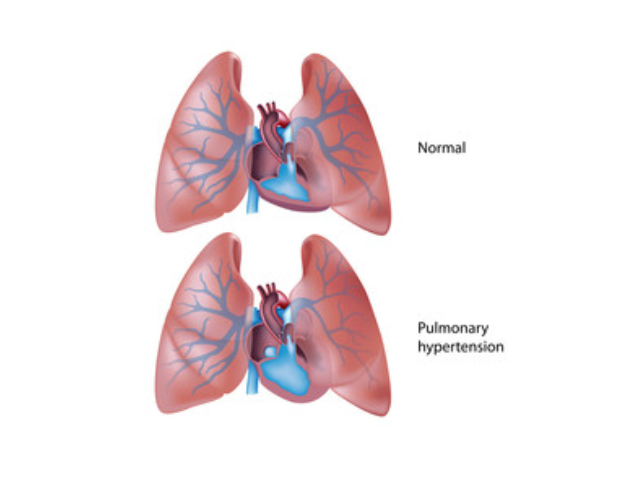
Pulmonary embolectomy is a surgical procedure that removes a blood clot from the pulmonary artery. The pulmonary artery is the main blood vessel that carries oxygenated blood from the heart to the lungs.
Pulmonary Hypertension | Dr Raghu
© 2024, Dr. Raghu. All rights reserved. Design & Developed by AMSDigital.in
+91 95424 75650