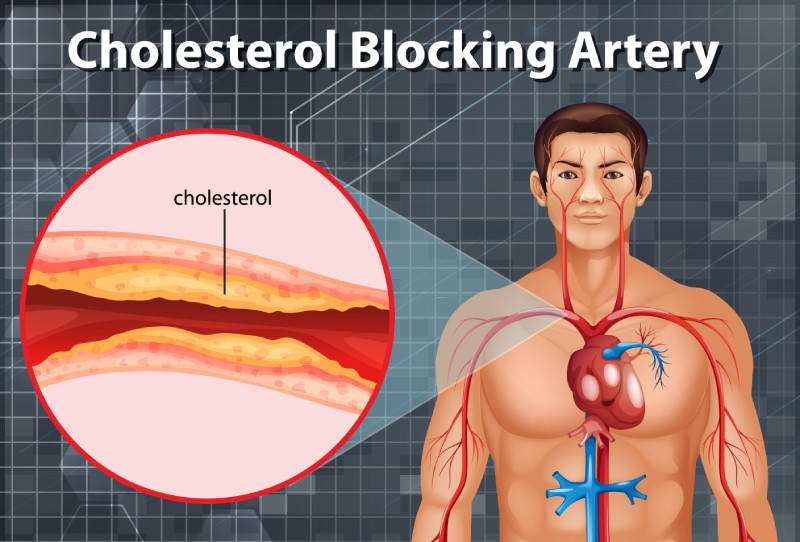
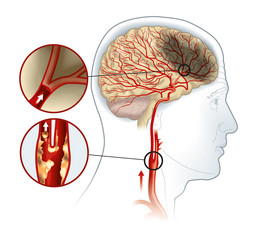
The Coronary Calcium Score is a measure of the amount of calcium deposits in the coronary arteries, which are the blood vessels supplying the heart.
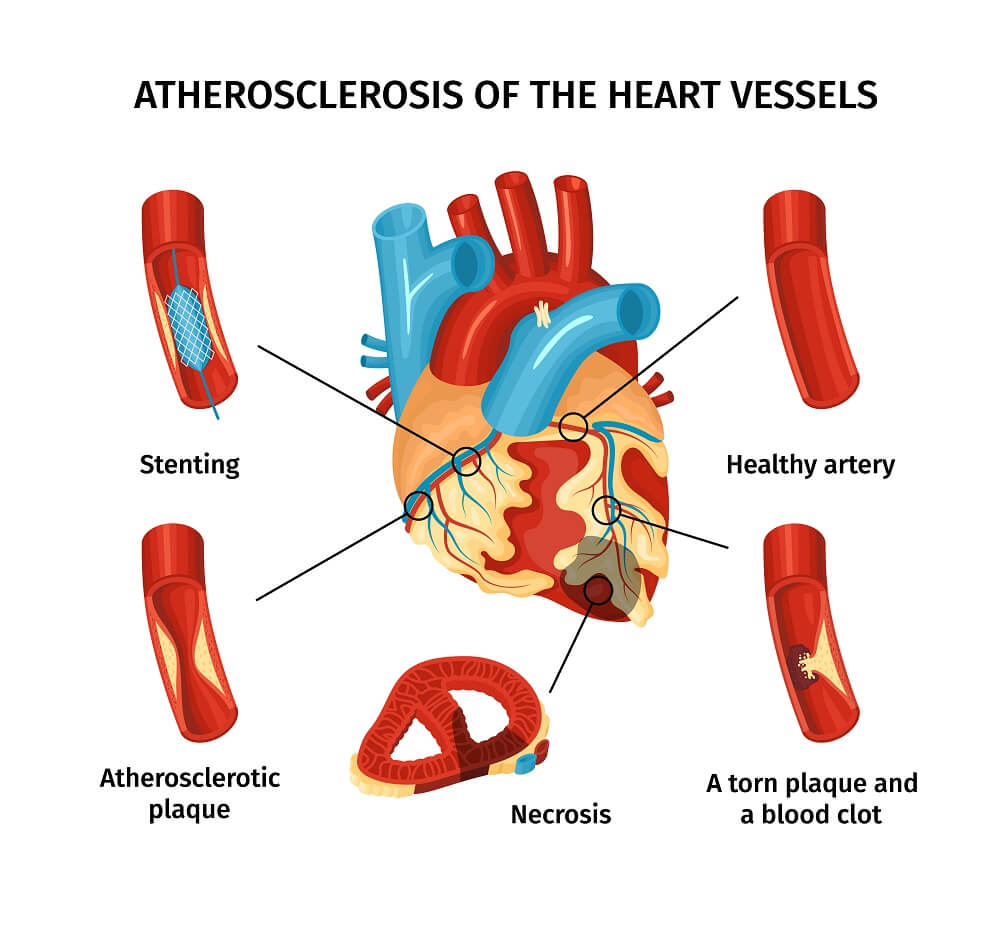
atherosclerosis | Dr Raghu
Cardiovascular diseases continue to be a leading cause of mortality globally, with calcified coronary arteries posing a significant challenge in interventional cardiology.
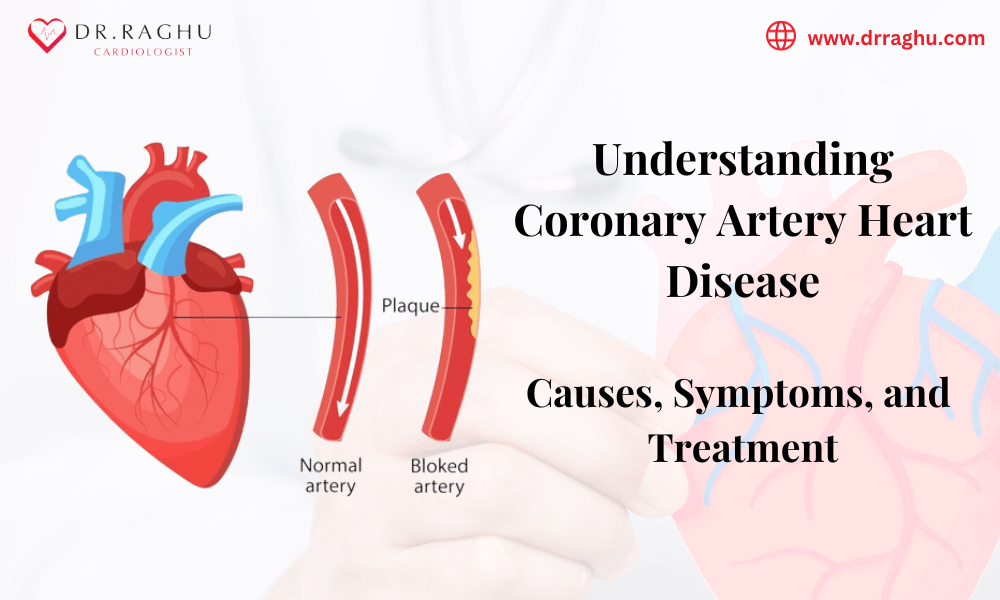
Coronary artery disease (CAD), commonly known as coronary heart disease or simply heart artery disease, is a prevalent and potentially life-threatening cardiovascular condition.
A heart attack, medically known as a myocardial infarction, is a severe medical emergency that can cause lasting damage to the heart muscle and even lead to death. As a leading cause of death worldwide, it shouldn't be taken lightly.
A heart attack, medically known as a myocardial infarction, is a severe medical emergency that can cause lasting damage to the heart muscle and even lead to death. As a leading cause of death worldwide, it shouldn't be taken lightly.
Heart disease is one of the major causes of death worldwide, and many factors increase its risk. These include high blood pressure, smoking, high cholesterol levels, obesity, physical inactivity...
Heart disease is a leading cause of death worldwide. Various factors, such as stress, underlying medical conditions, and a sedentary lifestyle, make an individual more vulnerable to heart disease.
The human body has two carotid arteries, on either side of the neck, that are responsible for carrying oxygen-rich blood to the brain and face. Plaque buildup in these arteries can lead to a condition called carotid artery disease.
Renal artery stenosis is a serious condition that can cause life-threatening complications if left untreated. It’s characterized by the narrowing of the renal arteries that carry oxygenated blood to the kidney.
Heart failure is a condition in which the heart can’t pump enough blood to meet the body’s needs. It’s a serious condition that requires treatment by your doctor, but there are several options available.