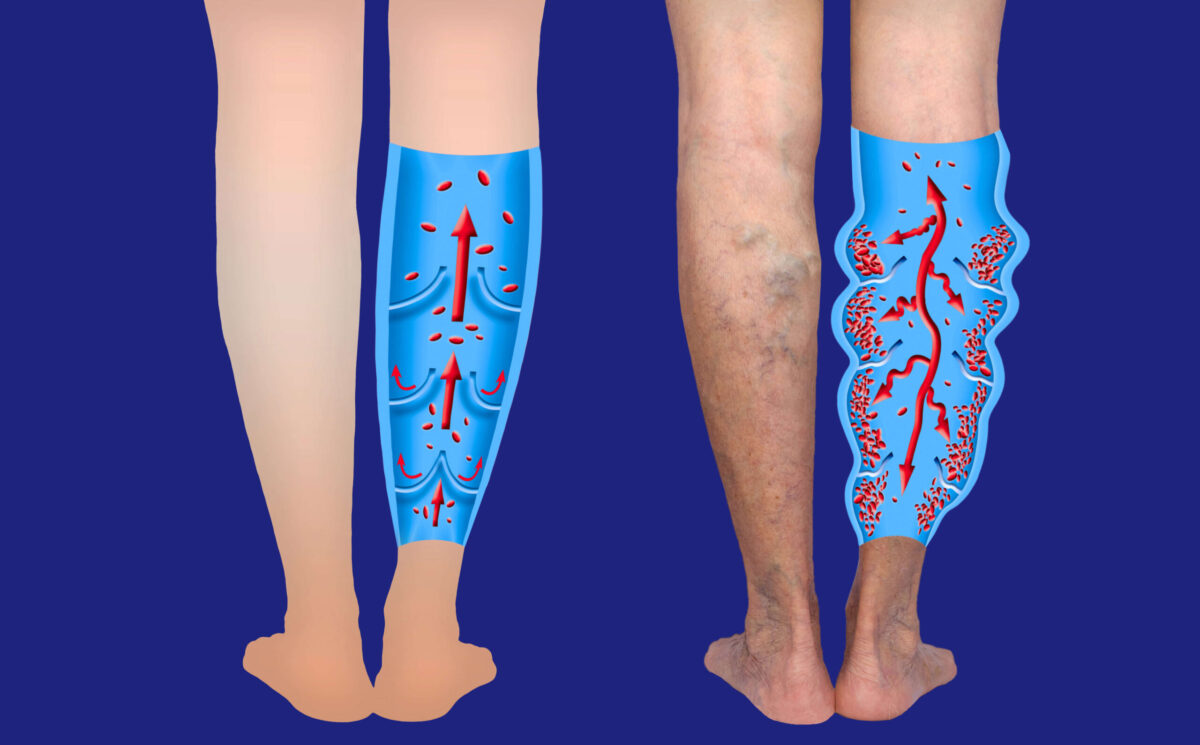
Venous insufficiency, or chronic venous insufficiency (CVI), is a condition where the veins stumble in their duty to return deoxygenated blood from the legs to the heart.
varicose veins | Dr Raghu
Venous insufficiency, or chronic venous insufficiency (CVI), is a condition where the veins stumble in their duty to return deoxygenated blood from the legs to the heart.
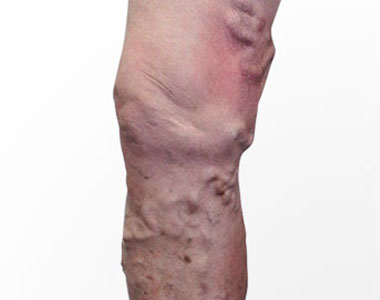
Varicose veins are the twisted, swollen and bulging veins that appear in blue, red and skin color, just beneath the surface of the skin. They occur mostly in the legs and feet, causing aching pain and discomfort in the legs.